You’ve been told it’s sciatica. You’ve tried stretching, maybe even seen someone about it, but the pain in your buttock won’t quit. It gets worse when you sit, worse when you climb stairs, and somehow worse after you’ve been walking for a while. Sound familiar?
There’s a decent chance it isn’t sciatica at all. It might be piriformis syndrome, a condition that mimics sciatica so closely that it gets misdiagnosed constantly. At Brooklyn Chiropractic Care, we find that roughly 6-8% of patients who come in thinking they have a disc problem are actually dealing with this instead [1]. Once we get the diagnosis right, it responds very well to treatment.
Key Takeaways
- Piriformis syndrome causes buttock and leg pain that looks almost identical to lumbar sciatica, but the source is a muscle, not a disc
- Pain gets worse with sitting, hip rotation, and climbing stairs, not typically with bending forward or coughing
- It accounts for 6-8% of all sciatica cases and is frequently misdiagnosed
- Chiropractic care, soft tissue therapy, and shockwave therapy are all effective without injections or surgery
- Mild cases resolve in 2-6 weeks. Chronic cases take 3-6 months with consistent treatment
What Is Piriformis Syndrome?
Piriformis syndrome is a condition where the piriformis muscle irritates the sciatic nerve, causing pain, numbness, or tingling that radiates from your buttock down the back of your leg.
The piriformis is a small, deep muscle that runs from your sacrum (the triangular bone at the base of your spine) to the top of your femur. It rotates your hip outward and helps stabilize the joint. The sciatic nerve runs directly behind it. In 15-37% of people, the nerve passes right through the muscle itself [1]. When the piriformis tightens, spasms, or swells, the sciatic nerve takes the hit.
Here’s the part that trips people up. The pain pattern is nearly identical to a herniated disc. Both cause buttock pain that radiates down the leg. But a disc problem starts in your spine. Piriformis syndrome starts in the muscle. They need completely different treatment approaches.
One pattern Dr. Patel sees often in our Greenpoint clinic: a patient comes in after months of failed sciatica treatment, MRI shows nothing significant, and within the first exam the piriformis is clearly the culprit. Not rare. Happens regularly.
What Causes Piriformis Syndrome?
Piriformis syndrome rarely comes from one moment. It usually builds over time. The most common causes we see in Brooklyn patients:
- Prolonged sitting. When you sit for hours, the piriformis stays shortened and compressed. Desk workers, drivers, and long subway commuters are especially prone. Symptoms often peak after a full workday or a long commute, not during activity.
- Overuse from running or cycling. These sports load the piriformis repeatedly through hip rotation. Distance runners and cyclists often develop this gradually, with no single injury to point to.
- Direct trauma to the buttock. A fall onto the hip or a car accident with impact to the seat can inflame or damage the piriformis directly. Post-accident piriformis syndrome is something we see in no-fault cases regularly.
- Weak glutes. When the gluteal muscles aren’t doing their job, the piriformis overcompensates to stabilize the hip. It gets overloaded. Eventually it protests.
- Anatomical variation. In a significant portion of the population, the sciatic nerve passes through or around the piriformis in an atypical path [1]. These people are more sensitive to even minor tightness in the muscle.
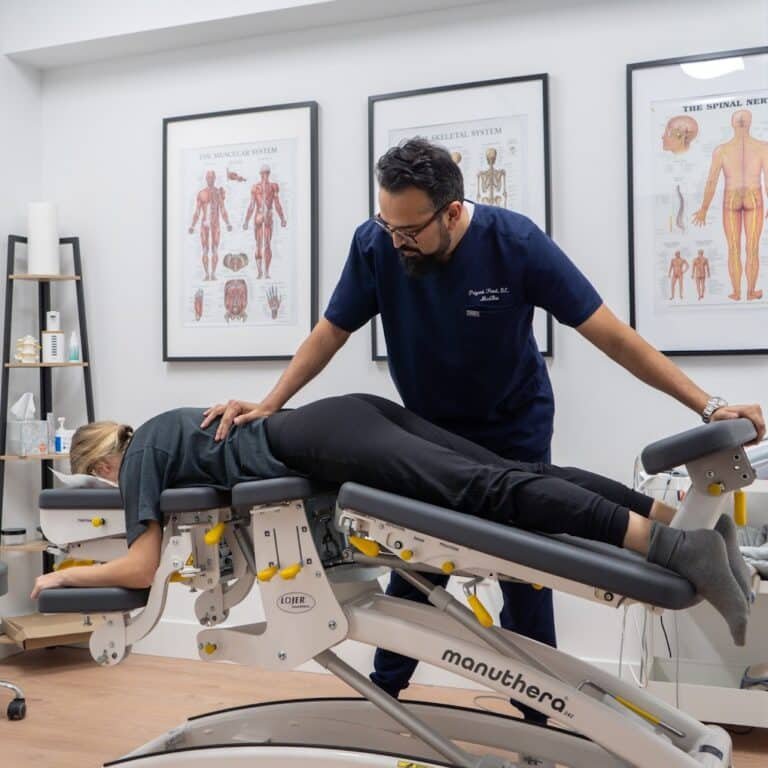
How Dr. Patel Treats Piriformis Syndrome
Getting the right diagnosis is the first step, and it requires more than an X-ray. X-rays don’t show piriformis syndrome. MRI often looks normal too [1].
At Brooklyn Chiropractic Care, Dr. Patel assesses your hip range of motion, performs the FAIR test (Flexion, Adduction, Internal Rotation), and palpates the piriformis to reproduce your symptoms. This clinical picture tells us what imaging can’t.
Once confirmed, treatment includes:
- Sacral and lumbar spinal manipulation. Restoring proper motion to the sacroiliac joint and lumbar spine reduces the mechanical load on the piriformis. Published research shows that chiropractic spinal manipulation combined with soft tissue work leads to full symptom resolution in piriformis syndrome cases [2].
- Soft tissue therapy on the piriformis directly. Trigger point work and myofascial release break the spasm cycle. For most patients, this is the part of treatment that brings the most immediate relief.
- Shockwave therapy for stubborn cases. A 2023 randomized controlled trial compared radial shockwave therapy to corticosteroid injection in 35 piriformis syndrome patients. Both produced significant pain reduction and quality of life improvement by 12 weeks. Shockwave showed faster early relief, with significant pain reduction at week one compared to no early change in the injection group [3]. That’s a non-invasive option that performs on par with injections. You can learn more about our shockwave therapy service in Brooklyn.
- Glute strengthening and hip stability work. Correcting the muscle imbalances that put the piriformis in an overworked position in the first place.
Mild cases that get treated early often resolve within 2-6 weeks. Chronic presentations, where the condition has been going on for months, typically need 3-6 months of consistent care. If you’ve been managing what seems like sciatica without real improvement, this diagnosis is worth exploring.
What to Expect During Your First Visit
Your first appointment is 45-60 minutes. It’s not just an adjustment.
Dr. Patel starts with your history. When did it start? What makes it worse? Have you had imaging? Then comes the physical exam: posture, gait, hip range of motion, and specific orthopedic tests. The FAIR test, Pace’s test, and direct palpation of the piriformis muscle give us more useful information than an MRI in most cases.
If piriformis syndrome is confirmed, you’ll likely get your first treatment that same day. More importantly, you’ll leave with a clear explanation of what’s actually happening and a realistic timeline for recovery. Not vague reassurance. A real plan.
Most patients notice some change after the first visit. Not full resolution, that takes time, but a shift in intensity or pattern that confirms you’ve found the right diagnosis and the right treatment.
Home Care: What You Can Do Between Visits
What happens between appointments matters. Here’s what actually works:
- Figure-4 piriformis stretch. Lie on your back. Cross your right ankle over your left knee. Gently pull your left thigh toward your chest until you feel a deep stretch in your right buttock. Hold 30 seconds, 3 sets per side, 3 times daily. This is the single most effective thing you can do at home.
- Clamshell exercise. Lie on your side with knees bent at 90 degrees and feet stacked. Keeping your feet together, rotate your top knee upward without letting your pelvis rock back. 3 sets of 15 reps per side, daily. Weak glutes are almost always part of what’s driving this condition.
- Break up sitting every 30-45 minutes. Stand up, walk to the other room, do a few bodyweight squats. Anything that interrupts the sustained hip flexion position that keeps the piriformis tight. Set a phone alarm if you need to.
- Ice for flares, then heat before stretching. During the first 48 hours of a flare-up, ice for 15 minutes to reduce inflammation. After that, apply moist heat for 15 minutes before your stretches to loosen the muscle first.
- Sleep with a pillow between your knees. Side-sleepers in particular: without support, your top hip drops into internal rotation all night. That’s hours of sustained piriformis irritation. A pillow between your knees keeps your hips neutral.
One mistake we see repeatedly: patients stretch aggressively during an active flare and make things worse. Gentle movement is fine during a flare. Aggressive stretching is not. If you’re unsure, ask Dr. Patel at your next visit before pushing through it.
Piriformis Syndrome: When to See a Doctor
Chiropractic care resolves the vast majority of piriformis syndrome cases without any need for injections or surgery. But some situations require a different level of care.
Get evaluated promptly if you have:
- Progressive leg or foot weakness, not just pain, but actual loss of strength
- Loss of bladder or bowel control
- Symptoms affecting both legs at the same time
- No improvement after 6 weeks of appropriate treatment
- Symptoms that began after significant trauma, a fall, or a car accident
These patterns can indicate something more serious: lumbar disc herniation with significant nerve compression, spinal stenosis, or in rare cases, a structural pathology that needs imaging and specialist involvement. If that’s the situation, we’ll tell you clearly and refer you appropriately. For ongoing back and hip pain that isn’t getting better, don’t keep waiting.
How do I know if I have piriformis syndrome or a herniated disc?
The clearest difference is what makes your pain worse. Piriformis syndrome gets worse with sitting, hip rotation, and climbing stairs. A herniated disc is typically worse with bending forward, coughing, or sneezing, and usually comes with lower back pain as well. The FAIR test and direct palpation of the piriformis during a clinical exam can differentiate between them. Imaging alone often can’t, since piriformis syndrome looks normal on MRI in many cases.
How long does piriformis syndrome take to heal?
Mild cases caught early resolve in 2-6 weeks with chiropractic care and consistent home exercises. Chronic cases that have been present for months typically take 3-6 months of treatment. The biggest variable is how long the condition has been active before treatment starts. Earlier is always faster.
Is sitting making my piriformis syndrome worse?
Yes. Prolonged sitting is one of the primary drivers of piriformis syndrome and one of the main reasons it doesn’t resolve on its own. When you sit, the piriformis is in a shortened, compressed position and the sciatic nerve is under tension. Breaking up sitting every 30-45 minutes is one of the most practical things you can do to support your recovery.
Does shockwave therapy actually work for piriformis syndrome?
Yes, with strong evidence. A 2023 randomized controlled trial found that radial shockwave therapy produced significant pain improvement at week one, faster than corticosteroid injection, with equivalent outcomes at the 12-week follow-up [3]. It’s a non-invasive, non-injection option that works well for cases that haven’t responded to manual therapy alone. We offer it at our Greenpoint clinic as part of a combined treatment plan.
Can I keep running while I’m being treated?
It depends on severity. Mild cases often tolerate reduced mileage with modified training: no hills, no speed work, shorter distances. Moderate-to-severe cases usually need a break from running to allow the muscle to recover. Dr. Patel will give you a specific recommendation based on what he finds, not a blanket answer.
Ready to find relief? Schedule an appointment online or visit us at Brooklyn Chiropractic Care, 112 Greenpoint Ave. STE 1B, Brooklyn, NY 11222.
References
- Hicks BL, Lam JC, Varacallo M. Piriformis Syndrome. StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Aug. Available from: https://www.ncbi.nlm.nih.gov/books/NBK448172/
- Boyajian-O’Neill LA, et al. Diagnosis and contemporary management of piriformis syndrome. J Am Osteopath Assoc. 2008;108(11):657-664.
- Haeri M, et al. Comparing radial extracorporeal shockwave therapy and corticosteroid injection in the treatment of piriformis syndrome: A randomized clinical trial. J Bodyw Mov Ther. 2023 Jan;33:182-188. PMID: 36775517.